-
What is a podiatrist?
posted: Sep. 17, 2018.

-
Movie actors
posted: Aug. 30, 2018.

-
Toe burned by garlic
posted: Jul. 29, 2018.

-
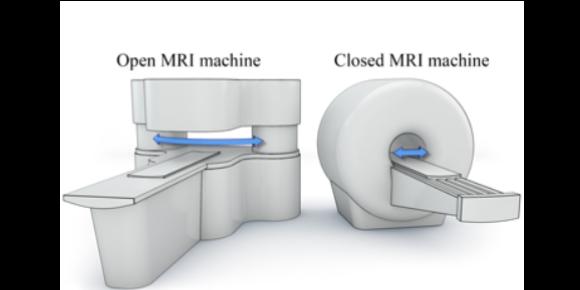
No yoga pants in MRI
posted: Jun. 14, 2018.
-
Plantar fibromatosis
posted: May 22, 2018.

-
Dad shoes
posted: Apr. 02, 2018.

-
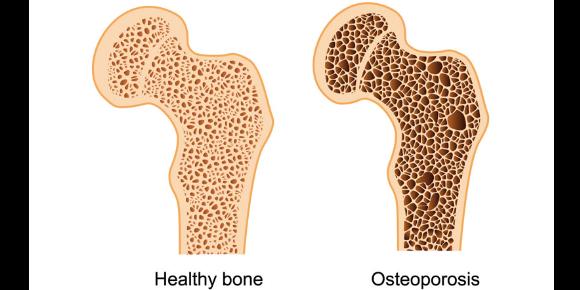
Osteoporosis
posted: Mar. 29, 2018.
-
Vitamins for strong bones
posted: Feb. 14, 2018.

-
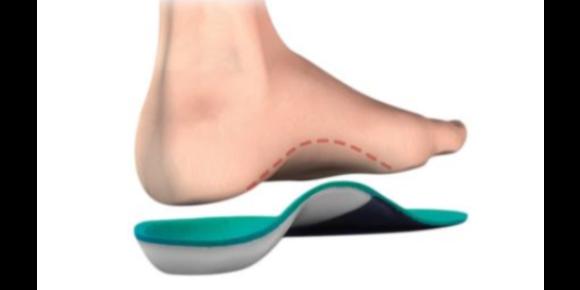
Orthotics
posted: Jan. 21, 2018.
-
Feet on dashboard is dangerous
posted: Dec. 25, 2017.

-
Forced to wear high heels
posted: Nov. 24, 2017.

-
Cool socks
posted: Oct. 19, 2017.

-
Hurrycane in office
posted: Sep. 08, 2017.

-
Largest NBA shoes
posted: Aug. 30, 2017.

-
Sneakers vs. tennis shoes
posted: Jul. 25, 2017.
What do you call the rubber-soled shoes that people wear during athletic activities? A New York Times questionnaire revealed that most Americans call them TENNIS SHOES. People in the Northeast USA Read more -
Diabetes medication
posted: Jun. 02, 2017.
Based on new data from clinical trials, the U.S. Food and Drug Administration (FDA) has concluded that a diabetes medication has an increased risk of amputation. Canagliflozin (known by the Read more